Natural Treatments for Pelvic Floor Dysfunction: How Acupuncture and Holistic Care Support Pelvic Health
Pelvic floor dysfunction is a problem of pelvic muscle tone and coordination that can cause pelvic pain, urinary leakage or urgency, constipation, and painful sex. Acupuncture and holistic care can support pelvic health by reducing muscle guarding, calming pain signaling, improving circulation, and helping the nervous system shift out of chronic fight-or-flight. The strongest non-surgical results typically come from combining acupuncture with pelvic floor physical therapy, plus targeted home habits that reduce pelvic pressure and retrain breathing and movement. Because these symptoms can feel private and exhausting, it is completely understandable to want a gentle, drug-free plan that helps you feel comfortable and in control of your body again.
Natural Treatments for Pelvic Floor Dysfunction: How Acupuncture and Holistic Care Support Pelvic Health
Pelvic floor dysfunction is a problem of pelvic muscle tone and coordination that can cause pelvic pain, urinary leakage or urgency, constipation, and painful sex. Acupuncture and holistic care can support pelvic health by reducing muscle guarding, calming pain signaling, improving circulation, and helping the nervous system shift out of chronic fight-or-flight. The strongest non-surgical results typically come from combining acupuncture with pelvic floor physical therapy, plus targeted home habits that reduce pelvic pressure and retrain breathing and movement. Because these symptoms can feel private and exhausting, it is completely understandable to want a gentle, drug-free plan that helps you feel comfortable and in control of your body again.
Key Takeaways
- Pelvic floor dysfunction is often a coordination issue, not just “weakness,” and many people have a tight-and-weak pattern.
- Acupuncture can reduce pain sensitivity and muscle guarding, which can make pelvic floor rehab easier and more tolerable.
- Pelvic floor physical therapy is a core treatment for retraining pelvic muscle timing, relaxation, and strength.
- Constipation prevention and bladder habit changes can significantly reduce pelvic floor strain and urgency loops.
- Seek urgent evaluation for sudden severe pelvic pain, fever, blood in urine, new saddle numbness, or new loss of bladder/bowel control.
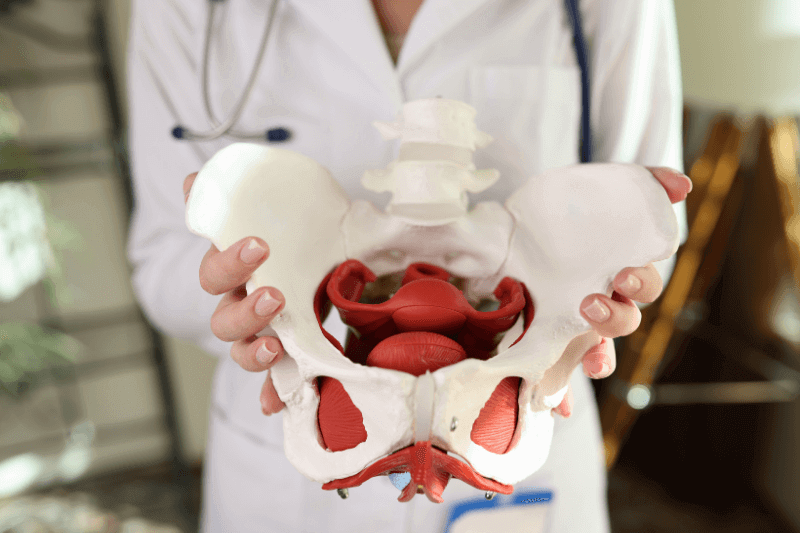
What is Pelvic Floor Dysfunction?
Pelvic floor dysfunction is a broad set of symptoms linked to abnormal pelvic floor muscle function, including muscles that are too tight, too weak, or poorly coordinated. It commonly involves problems with relaxing, contracting, or timing the pelvic floor correctly during urination, bowel movements, and sexual activity. Pelvic organ support changes can also be involved.
Types of Pelvic Floor Dysfunction
Pelvic floor dysfunction is not one single condition. It is a category that includes different muscle and nerve patterns, and the “type” matters because treatment changes depending on whether the pelvic floor needs to relax, coordinate better, or build strength.
1) Hypertonic Pelvic Floor Dysfunction (Overactive, Tight Pelvic Floor)
This type happens when the pelvic floor muscles stay contracted and struggle to fully release.
Common signs
- Pelvic pain, tailbone pain, or deep aching in the pelvis
- Urinary urgency or frequent urination (even when the bladder is not full)
- Constipation, straining, or feeling like you cannot fully empty
- Pain with sex or difficulty with penetration
- Muscle “guarding” that worsens with stress, sitting, or flare-ups
Why it happens
Stress-related tension, past pain or inflammation, trauma responses, posture and hip tightness, endometriosis-related pain, bladder irritation, or repeated straining can keep the pelvic floor stuck in a protective “on” state.
2) Hypotonic Pelvic Floor Dysfunction (Underactive, Weak Pelvic Floor)
This type happens when the pelvic floor muscles cannot generate enough strength or endurance to support the pelvic organs or maintain continence.
Common signs
- Urinary leakage with coughing, laughing, running, or lifting
- A sense of heaviness, pressure, or “falling out” sensations
- Early fatigue during activity or after long periods standing
- Reduced pelvic stability, sometimes with low back discomfort
Why it happens
Childbirth, aging-related tissue changes, hormonal changes (including menopause), connective tissue laxity, surgery, or long-term deconditioning can reduce pelvic support and muscle capacity.
3) Incoordination or Dyssynergic Pelvic Floor Dysfunction (Timing and Control Problem)
This type happens when the pelvic floor does not relax when it should, or it activates at the wrong time, even if it is not clearly “tight” or “weak” overall.
Common signs
- Straining even when stool is soft
- Feeling blocked during bowel movements
- Incomplete emptying (bowel or bladder)
- Alternating constipation and urgency patterns
- Symptoms that improve temporarily with position changes
Why it happens
Learned holding patterns, chronic constipation history, poor breathing mechanics, abdominal bracing, pain avoidance, or nervous system dysregulation can disrupt the normal “relax-then-contract” sequence.
4) Mixed Pelvic Floor Dysfunction (Tight-and-Weak Pattern)
This is one of the most common real-world presentations: the pelvic floor is tight in some areas but weak or poorly recruiting in others.
Common signs
- Pain plus leakage (or urgency plus heaviness)
- Symptoms that worsen with “random Kegels”
- Tight hips, shallow breathing, and core bracing
- Relief when tension is released, but symptoms return without retraining
Why it matters
This type needs the right order: down-train tension first, then rebuild coordination and strength. Strengthening too early can lock in guarding and worsen symptoms.
5) Myofascial Pelvic Floor Dysfunction (Trigger Point-Driven Pelvic Pain)
This type is driven by sensitive trigger points and fascial restrictions in pelvic floor muscles and nearby structures (hips, glutes, obturator internus, adductors).
Common signs
- Referred pain (vaginal, rectal, bladder, groin, or low back pain)
- Pain with sitting, penetration, tampon use, or pelvic exams
- Burning, aching, or “electric” discomfort without infection
- Pain that flares with stress and improves with manual release
Why it happens
Chronic guarding, past injury, surgery, inflammation, postpartum strain, and repetitive sitting or athletic overuse can create trigger-point patterns.
6) Neurogenic Pelvic Floor Dysfunction (Nerve Irritation and Sensitization Component)
In some cases, pelvic symptoms are strongly influenced by nerve irritation or heightened nervous system sensitivity, especially in chronic pelvic pain conditions.
Common signs
- Burning, sharp, or radiating pain
- Pain that lingers long after the original trigger
- Hypersensitivity to touch or pressure
- Symptoms that flare with stress, poor sleep, or prolonged sitting
Why it matters
This type often responds best to a nervous-system-informed plan: pain modulation, down-training, gentle graded exposure, and coordinated care (PT + acupuncture + medical evaluation when needed).
Pelvic Floor Dysfunction in Men
Pelvic floor dysfunction can affect men when the pelvic muscles are too tight, too weak, or poorly coordinated, leading to urinary, bowel, sexual, and pelvic pain symptoms. In men, it often overlaps with chronic pelvic pain syndrome and “prostatitis-like” symptoms without infection.
Common symptoms in men
- Urinary urgency/frequency, hesitancy, weak stream, post-void dribbling
- Pelvic, perineal, tailbone, groin, testicular, or penile pain (often worse with sitting)
- Constipation, straining, or difficulty fully emptying
- Pain with ejaculation, reduced sexual comfort, or erectile issues linked to pain/tension
Why it happens
Common drivers include stress-related muscle guarding, prolonged sitting or cycling pressure, hip/core tightness, constipation and straining, prior pelvic procedures, and nervous system sensitization.
What helps naturally
The most effective conservative approach typically combines pelvic floor physical therapy (down-training, coordination retraining, manual therapy, biofeedback) with supportive acupuncture for pain modulation and muscle relaxation, plus breathwork and bowel/bladder habit changes.
Why Whole-Person Care Works Better Than One Isolated Fix
The pelvic floor is not a standalone muscle group. It is part of a pressure and stability system that includes the diaphragm, abdominal wall, spine, hips, and nervous system. When stress, pain, constipation, posture, or breathing mechanics are off, the pelvic floor often compensates by gripping or collapsing.
A practical way to think about it:
- Pain and threat signals increase guarding.
- Guarding increases pain and urinary urgency.
- Avoidance and poor mechanics weaken coordination over time
Breaking that loop usually takes more than one tool.
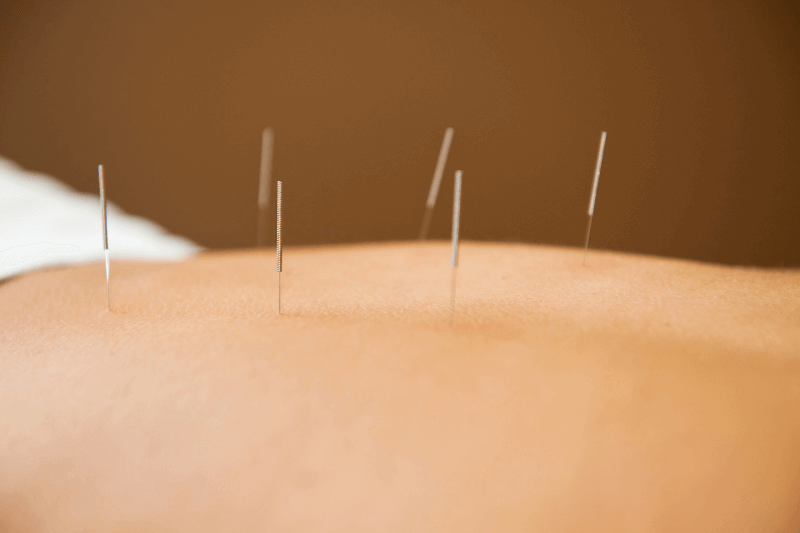
How Acupuncture Supports Pelvic Health
Acupuncture can support pelvic floor dysfunction by reducing pain sensitivity, decreasing muscle guarding, and shifting the nervous system toward calmer regulation. It may also support local circulation and recovery, especially when pain and tension are the dominant drivers. In many care plans, it is used as a catalyst that makes pelvic floor rehab possible.
1) Muscle relaxation and “de-guarding”
In hypertonic presentations, the immediate win is often reduced protective tension. When muscles stop clenching reflexively, urination, bowel movements, and intimacy can become less painful and less “restricted.” Hypertonic pelvic floor symptoms commonly include pain plus difficulty with urination, bowel movements, and sexual function, which is why de-guarding is a meaningful target.
2) Pain modulation and calmer signaling
Acupuncture is frequently discussed in terms of endorphin release and altered pain processing. Clinically, the relevant outcome is simpler: lower pain amplification helps people move, breathe, and participate in pelvic floor PT more consistently.
3) Circulation support in the pelvic basin
Improved microcirculation is often proposed as a mechanism for pelvic tissue recovery and for “congestion” sensations. This is most useful as supportive language, not a promise of cure, especially in complex conditions.
4) Nervous system regulation (stress and pelvic symptoms are linked)
Many pelvic floor disorders flare when the nervous system is stuck in high-alert mode. The pelvic floor is a common “bracing” site during chronic stress, trauma responses, or persistent pain. A plan that improves sleep, reduces vigilance, and softens guarding is often a turning point.
5) Hormone-axis support, with clear boundaries
Some integrative models describe acupuncture as supporting hypothalamic-pituitary-gonadal axis regulation and hormonal balance. It is best framed as supportive, not as a replacement for medical evaluation when symptoms suggest endometriosis, fibroids, infection, or significant bleeding changes.
Acupuncture Strategy by Pelvic Floor Pattern
If your pelvic floor is tight and painful (hypertonic pattern)
These are common goals:
- reduce guarding and trigger-point sensitivity
- improve bladder and bowel ease
- down-train urgency and pelvic pain flares
- improve sleep quality and stress reactivity
Hypertonic pelvic floor is a recognized pattern with pain and functional difficulty (urinary, bowel, sexual).
If your pelvic floor is weak or leaky (hypotonic pattern)
Acupuncture is typically used as support, while the cornerstone becomes:
- recruitment training
- endurance building
- functional strength that matches real life, coughing, lifting, running
If you are “tight and weak” (the common reality)
Many people have both guarding and poor recruitment. In those cases, the sequence matters:
- down-train and restore mobility
- retrain coordination
- build strength and endurance
Where electroacupuncture may fit
Electroacupuncture is often studied in continence contexts and may be considered as part of an integrative protocol, especially when paired with pelvic muscle training and objective tracking.
The Highest-Leverage Combination: Pelvic Floor PT + Acupuncture
Pelvic floor physical therapy is a core evidence-based approach for many pelvic floor problems, using strategies like biofeedback training, manual techniques, and behavior modification to retrain pelvic floor function.
Why pairing helps:
- Pelvic floor PT retrains mechanics, timing, and strength.
- Acupuncture can reduce pain and guarding so the PT work is tolerable and consistent.
Biofeedback matters because it makes the invisible visible. It helps people learn what “relax” and “engage” actually feel like, which is critical for both hypertonic and hypotonic patterns.
Integrative Therapies That Strengthen Results (And Keep Them)
A holistic plan is not a mix of random modalities. It targets the drivers that keep the pelvic floor tense, irritated, or poorly coordinated.
- Myofascial and trigger-point work: Often used to reduce muscle knots and pelvic pain patterns, especially in chronic pelvic pain.
- Breathwork and pressure management: Diaphragmatic breathing helps coordinate the diaphragm and pelvic floor so you are not bracing or straining all day.
- Mindful movement: Yoga, Pilates, tai chi, and qigong can improve alignment, hip function, and the ability to both relax and engage the pelvic floor.
- Supportive levers: Heat may ease guarding, sleep improves pain resilience, and magnesium may support muscle relaxation when appropriate.
Diet, Digestion, and Bladder Habits That Protect the Pelvic Floor
Pelvic symptoms often improve when daily strain is reduced.
- Constipation prevention: Fiber, hydration, and better toileting posture reduce straining and pelvic pressure.
- Bladder triggers: Identifying irritants like caffeine, carbonation, and acidic drinks can reduce urgency, especially when paired with bladder retraining strategies.
What to Expect From Treatment
A typical acupuncture session for pelvic health often runs about 45 to 60 minutes, with a plan tailored to symptoms and pattern. Many people notice early changes in sleep quality, pain flare intensity, and urgency within the first few sessions, but durable change usually requires consistency plus retraining and habit shifts.
A practical 6 to 12 week framework
- Weeks 1 to 3: reduce guarding, improve sleep, improve bowel and bladder ease
- Weeks 4 to 8: coordination retraining and graded strengthening or relaxation protocols
- Weeks 9 to 12: consolidate with functional movement, lifting mechanics, relapse prevention
Safety and Red Flags
Natural care should never delay medical evaluation when symptoms suggest infection, bleeding disorders, neurologic compromise, or acute pelvic pathology.
Seek urgent care for:
- fever with pelvic pain
- blood in urine
- sudden severe pelvic pain
- new saddle numbness
- new loss of bladder or bowel control
Supportive, Personalized Care That Adapts as You Improve
Pelvic floor symptoms often shift over time, which is why the most helpful care is personalized and responsive rather than one-size-fits-all. Our practitioners take time to understand your symptom pattern and goals, then tailor acupuncture and holistic care to support muscle regulation, pain relief, and nervous system balance. Depending on what is appropriate for your presentation, supportive services may also include gentle bodywork, moxibustion, and cupping, along with practical lifestyle guidance for stress, sleep, digestion, and bladder habits. If you would like a plan built around your needs, you can contact us at ACA Acupuncture and Wellness to schedule a visit.
Sources:
Ding, S. (2023). Integrative medicine for pelvic floor disorders: A conceptual framework. Gynecology and Obstetrics Clinical Medicine, 3(3), 140–143.
Srinivasan, M., Torres, J. E., McGeary, D., & Nagpal, A. S. (2020). Complementary and alternative (CAM) treatment options for women with pelvic pain. Current Physical Medicine and Rehabilitation Reports, 8(3), 240–248.
Frequently Asked Questions
Can acupuncture fix pelvic floor dysfunction?
Acupuncture can help pelvic floor dysfunction by reducing pelvic pain, easing muscle guarding, and supporting calmer nervous system regulation. It is most effective when it makes pelvic floor physical therapy easier to tolerate and more consistent, especially in tight or pain-dominant patterns. Long-term improvement usually comes from pairing acupuncture with pelvic PT and daily home retraining for coordination, breathing, and pressure control.
Is pelvic floor dysfunction always weak muscles?
No, pelvic floor dysfunction is often a tone and coordination problem, not just weakness. Some people have an overactive pelvic floor that cannot relax, while others have underactive muscles that lack support or endurance. Many cases are “tight-and-weak,” so treatment must match the pattern to avoid worsening symptoms.
Can acupuncture help urinary incontinence or overactive bladder?
Acupuncture can support continence goals by reducing urgency-related nervous system overactivity and improving pelvic muscle regulation. It is typically used alongside pelvic floor muscle training, bladder retraining, and pelvic health physical therapy rather than as a stand-alone fix. Outcomes are best when treatment is consistent and progress is tracked with symptom changes like fewer leaks or reduced frequency.
Can acupuncture help postpartum pelvic floor recovery?
Acupuncture can support postpartum recovery by easing pelvic pain, calming stress-driven tension, and improving comfort so rehab is easier to follow. It is commonly combined with pelvic floor physical therapy to rebuild coordination, strength, and pressure management after pregnancy and delivery. The best plans are individualized, especially if symptoms include leakage, heaviness, or painful sex.
Can pelvic floor dysfunction cause back pain?
Yes, pelvic floor dysfunction can contribute to low back, sacral, or tailbone pain because the pelvic floor works with the core, hips, and diaphragm to stabilize the spine. Tight pelvic muscles can create pulling and guarding patterns that refer pain into the lower back, while weakness or poor coordination can force other muscles to overcompensate. Back pain that changes with sitting, bowel movements, or urinary symptoms can be a clue the pelvic floor is involved.
How is pelvic floor dysfunction diagnosed?
Diagnosis starts with a symptom review and a focused exam to assess pelvic floor muscle tone, strength, coordination, and the ability to relax. A pelvic health physical therapist or qualified clinician may also evaluate breathing mechanics, posture, hip function, and how the pelvic floor responds during bearing down and contraction. Biofeedback, ultrasound, or other tests may be used when needed, and clinicians often rule out infections, gynecologic/urologic conditions, or neurologic red flags.
Contact ACA Acupuncture & Wellness
Get in Touch
Newsletter Sign Up
LOCATIONS
MANHATTAN
QUEENS
NEW JERSEY
CALIFORNIA

ACA Franchise Opportunities
The over $4 billion US acupuncture market offers a great opportunity with over 10% annual growth rates and a continuing flow of new patients interested in the benefits of acupuncture.